 serum creatinine value depends on the assay method and calibration used.Moreover, there is creatininemia fluctuation in those cirrhotic patients with refractory ascites and/or those receiving diuretics ( 5, 12- 16) the muscle mass, protein intake, age, gender and ethnicity, can also influence serum creatinine levels.Since creatinine is synthesized in the liver, any cause of hepatic parenchymal dysfunction will reduce its production, leading to a markedly lower serum creatinine levels compared to general population ( 11, 13) serum creatinine is an inaccurate renal functional marker in the majority of cirrhotic patients since creatinine generation and excretion are usually modified in cirrhotic individuals.Even though, the MELD score has been widely validated in different populations of cirrhotic patients, and serum creatinine has a significant prognostic value in this group, even better than liver functional markers themselves ( 1, 10, 11), it has been suggested that creatinine weighs too heavily on this score, being a variable which has some concerns, such as ( 1, 10- 16): In practice, a MELD score of 15 is now considered as the limit above which a liver transplantation should be considered (except when hepatocarcinoma is present) ( 6- 9). Even though, the MELD score is the criterion to prioritize patients for liver allocation, the presence of ascites (and its severity) is a well-known determinant of glomerular filtration rate (GFR) due to hemodynamic mechanisms. Recently, MELD-Na has been proposed as an alternative to MELD for liver transplant allocation due to the inverse association between serum sodium and short-term survival on the waiting list ( Table 2) ( 4, 5). MELD, model for end-stage liver disease IRN, international normalized ratio. It is worth mentioning that since MELD score was introduced, increased utilization of combined kidney and liver transplants without a significant change in post-transplant survival has been reported ( 3- 6). The three variables included by this score, which are two hepatic (serum bilirubin and one international normalized ratio) and one renal (serum creatinine), highlight the prognostic significance of the interactions between liver and renal functions in cirrhotic patients ( Table 1) ( 1- 5). The MELD score accurately predicts short-term mortality on the liver transplant waiting list. Thus, the Model for End-stage Liver Disease (MELD) score was developed as a simple, and more objective hepatic score compared to Child-Pugh score ( Table 1) ( 1- 3). However, the Child-Pugh score has the limitations of the subjective interpretation of ascites and encephalopathy. This score is based on five variables: ascites, encephalopathy, serum bilirubin, serum albumin and prothrombin time, which was empirically selected, and has been proved to be a reliable prognostic tool in many clinical situations ( 1, 2). Conclusion: despite some concerns, MELD score is currently useful for guiding liver transplant allocation.įor many decades the Child-Pugh score has been the main prognostic tool for cirrhotic patients. The MELD score has been widely validated in different populations of cirrhotic patients, but it has been suggested that creatinine weighs too heavily on this score. Recently, MELD alternative forms (sodium MELD, and corrected creatinine MELD), and its combination with estimated glomerular filtration rate (eGFR), have been proposed as more reliable markers. It accurately predicts short-term mortality on the liver transplant waiting list, and its three variables: serum bilirubin, creatininemia, and international normalized ratio, highlight the prognostic significance of the interactions between liver and renal functional variables in cirrhotic patients. The Model for End-stage Liver Disease (MELD) score was developed as a simple, and more objective hepatic score compared to Child-Pugh. Received: 11 October 2017 Accepted: 27 October 2017 Published: 18 November 2017. 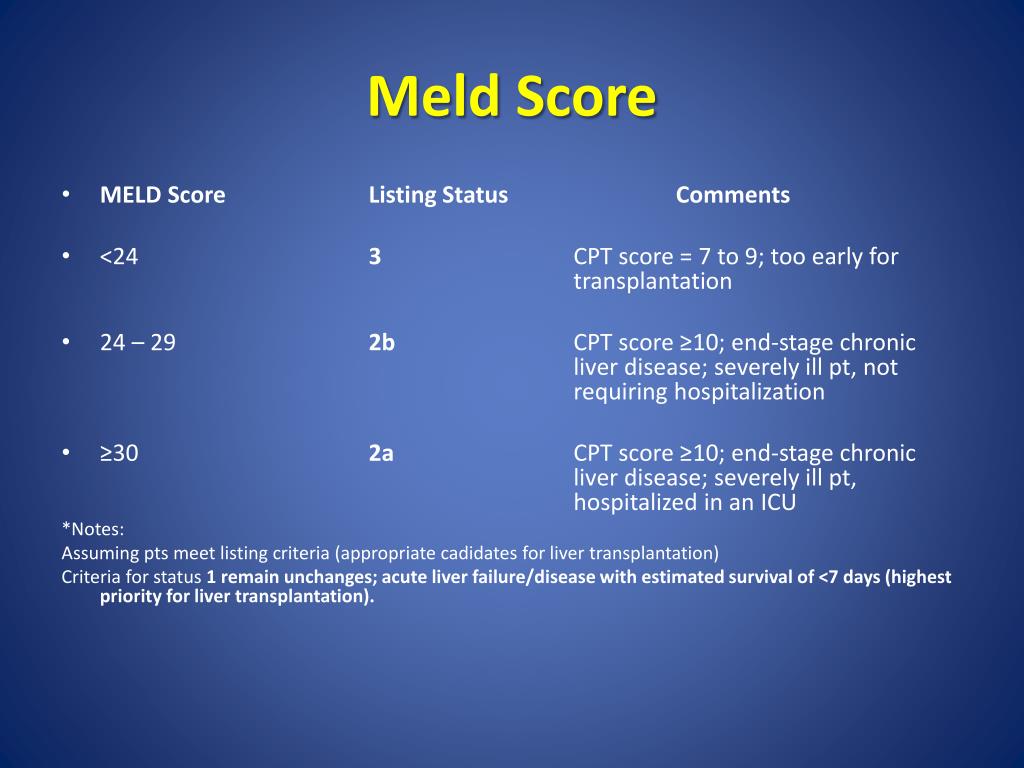
Acute kidney injury in cirrhosis: baseline serum creatinine predicts patient outcomes. Email: on: Wong F, O‘Leary JG, Reddy KR, et al. Human Physiology Department, Instituto Universitario del Hospital Italiano de Buenos Aires, Argentina.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
